Stopping edibles before surgery is a critical safety step that protects against anesthesia complications, uncontrolled bleeding, and unpredictable drug interactions during any procedure.
This guide covers the pharmacological reasons surgeons require cannabinoid cessation, specific timelines for different edible types and procedures, surgical risks of noncompliance, the importance of honest provider disclosure, safer pre-surgery alternatives, cannabinoid clearance windows, and post-operative resumption guidelines.
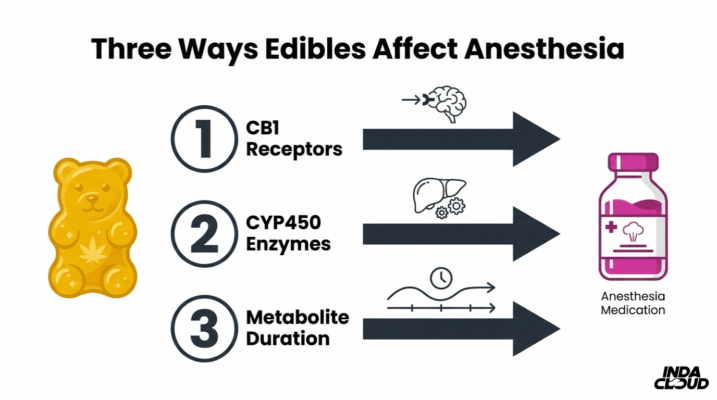
Cannabinoids from edibles interact with anesthesia through multiple mechanisms. THC desensitizes CB1 receptors in chronic users, while both THC and CBD inhibit the CYP450 liver enzymes responsible for metabolizing surgical medications. Edibles pose a distinct challenge because oral THC converts into 11-hydroxy-THC, a more potent, longer-lasting metabolite than what inhaled cannabis produces.
Cessation timelines vary by cannabinoid and procedure type. THC edibles generally require a minimum 72-hour pause before general anesthesia, with heavier users benefiting from one to two weeks of abstinence. CBD edibles warrant 48 to 72 hours, delta-8 products need 72 hours to one full week, and cosmetic surgery often demands the longest window at one to two weeks due to heightened bleeding and healing concerns.
Consuming edibles too close to surgery increases the risk of anesthesia resistance, cardiovascular instability, excessive bleeding, dangerous drug accumulation, and worsened postoperative nausea. Disclosing all cannabinoid use to your surgical team remains essential, since nearly half of cannabis users withhold this information from providers despite the serious safety implications.
Evidence-based alternatives for pre-surgery anxiety include cognitive-behavioral therapy, music therapy, guided imagery, acupuncture, and doctor-prescribed anxiolytics. After medical clearance, quality lab-tested hemp edibles from brands like IndaCloud can reenter a wellness routine at conservative doses aligned with your recovery stage.
Why Do Surgeons Ask You to Stop Using Edibles Before Surgery?
Surgeons ask you to stop using edibles before surgery because cannabinoids interfere with anesthesia, increase bleeding risk, and complicate recovery. The American College of Surgeons recommends that patients stop using marijuana products at least 72 hours before surgery to reduce the risk of breathing problems. THC and CBD affect the same enzyme systems that metabolize surgical medications, creating unpredictable drug interactions. Cannabinoids also influence heart rate, blood pressure regulation, and airway responsiveness, all of which anesthesiologists must carefully control during a procedure. For patients who use edibles regularly, these effects can be more pronounced because cannabinoids accumulate in fat tissue and remain active longer than many realize. Honest disclosure to your surgical team allows them to adjust protocols and keep you safer on the operating table.
How Do Cannabis Edibles Interact with Anesthesia?
Cannabis edibles interact with anesthesia by altering how the body processes anesthetic drugs, affecting sedation depth, pain response, and cardiovascular stability. THC, CBD, and their metabolites each create distinct challenges during surgery.
How Does THC Affect General Anesthesia?
THC affects general anesthesia by activating CB1 receptors in the brain and central nervous system, which can alter sedation depth and pain signaling. Chronic cannabis use causes down-regulation and desensitization of these CB1 receptors, a process that begins reversing after 24 to 48 hours of abstinence and normalizes in approximately four weeks, according to research published in Regional Anesthesia & Pain Medicine. This receptor tolerance means regular THC users may respond unpredictably to standard anesthetic doses. Anesthesiologists often need to adjust their protocols, since blunted CB1 receptor activity can reduce the effectiveness of agents that rely on similar neurological pathways. For patients who consume edibles regularly, this tolerance effect is particularly relevant because oral THC produces sustained cannabinoid exposure.
How Does CBD Affect Sedation and Anesthesia Medications?
CBD affects sedation and anesthesia medications primarily through its interaction with the CYP450 enzyme system. THC and CBD are both metabolized extensively by CYP450 enzymes and also inhibit many of these enzymes, potentially leading to variable serum concentrations of other drugs, as noted by the National Institutes of Health. Because many anesthetic agents, sedatives, and analgesics depend on CYP450 for metabolism, CBD can slow their breakdown and increase their effective concentration in the bloodstream. This enzyme inhibition may prolong sedation or amplify side effects from medications administered during surgery. Even patients who use CBD-only products without THC should disclose this to their surgical team, since the enzyme interaction alone presents a meaningful clinical concern.
How Do Edibles Differ from Smoked Cannabis in Anesthesia Risk?
Edibles differ from smoked cannabis in anesthesia risk because of their distinct pharmacokinetic profile. The bioavailability of inhaled THC ranges from 10% to 35%, whereas oral THC from edibles is only 4% to 12% bioavailable due to extensive first-pass hepatic metabolism, according to research published in the National Institutes of Health. Although edibles deliver less THC per milligram consumed, first-pass metabolism converts oral THC into 11-hydroxy-THC, a more potent and longer-lasting metabolite. This means edibles produce prolonged cannabinoid activity that can complicate anesthesia timing in ways smoking does not.
Key differences include:
- Edibles produce delayed onset (30 to 90 minutes) and extended duration (6 to 12 hours), making residual effects harder to predict before surgery.
- Smoked cannabis poses acute cardiovascular risks; ASRA guidelines recommend delaying elective surgery a minimum of two hours after smoking.
- ASRA consensus-based guidelines recommend reducing cannabinoid use 7 days before surgery to under 300 mg per day for edibles or 1.5 g per day for smoked cannabis.
- Daily cannabis use is associated with a 3.3% absolute marginal increase in postoperative nausea and vomiting risk.
The prolonged metabolite activity from edibles makes accurate pre-surgical timing more critical than with inhaled forms, which is why many anesthesiologists consider edibles the more complex variable to manage perioperatively.
How Long Before Surgery Should You Stop Taking Edibles?
You should stop taking edibles at least 72 hours before surgery, though timelines vary by cannabinoid type and procedure. The following subsections break down cessation periods for THC edibles, CBD edibles, delta-8 products, dental surgery, and cosmetic surgery.

How Long Should You Stop THC Edibles Before General Anesthesia?
You should stop THC edibles before general anesthesia at least 72 hours in advance, with heavier users benefiting from a longer cessation window of one to two weeks. THC edibles produce 11-hydroxy-THC during digestion, a metabolite more potent and longer-lasting than inhaled delta-9-THC. This extended metabolic activity increases the risk of anesthesia resistance, cardiovascular instability, and postoperative nausea.
According to the American Society of Regional Anesthesia and Pain Medicine (ASRA), all patients should be screened for cannabis use before surgery, noting that regular use may worsen pain and nausea. Chronic daily users should taper gradually rather than stop abruptly, as sudden cessation can trigger withdrawal symptoms that complicate the surgical experience. Always disclose your full edible history to your anesthesiologist for the safest dosing adjustments.
How Long Should You Stop CBD Edibles Before Surgery?
You should stop CBD edibles before surgery at least 48 to 72 hours in advance. Although CBD is non-intoxicating, it inhibits CYP450 liver enzymes responsible for metabolizing many surgical medications, including sedatives, blood thinners, and anesthetics. This enzyme inhibition can cause unpredictable drug levels during and after a procedure.
CBD’s effects on platelet aggregation also raise concerns about bleeding risk. Patients taking CBD alongside prescription blood thinners face compounded anticoagulant effects that surgeons need to account for. Even if your CBD edibles contain less than 0.3% THC, the enzyme interaction alone warrants a pre-surgical pause. Inform your surgical team about dosage, frequency, and the specific CBD products you use so they can plan accordingly.
How Long Should You Stop Delta-8 Edibles Before a Procedure?
You should stop delta-8 edibles before a procedure at least 72 hours to one week prior. Delta-8-THC behaves similarly to delta-9-THC in the body, binding to CB1 receptors and producing psychoactive effects, yet it carries distinct metabolic risks. A study published in the National Institutes of Health (PMC) found that delta-8-THC results suggest a high risk of drug interactions, especially with oral use, due to its inhibitory effects on major hepatic enzymes.
Because delta-8 edibles undergo the same first-pass liver metabolism as other oral cannabinoids, they generate active metabolites that persist longer than inhaled forms. For anyone using delta-8 daily, a full seven-day cessation period is the more cautious approach before any procedure requiring sedation or anesthesia.
How Long Should You Stop Edibles Before Dental Surgery?
You should stop edibles before dental surgery at least 48 to 72 hours in advance. Dental procedures often involve local anesthesia, nitrous oxide sedation, or IV conscious sedation, all of which can interact with cannabinoids in your system. THC edibles may reduce the effectiveness of local anesthetics, potentially requiring higher doses to achieve adequate numbing.
Cannabinoids can also increase heart rate and alter blood pressure, complicating sedation monitoring during longer procedures like wisdom tooth extractions or implant placements. Oral tissues may experience prolonged bleeding when cannabinoids interfere with platelet function. For procedures under general anesthesia, such as complex oral surgeries, extending your cessation window to a full week offers a wider safety margin. Disclose all edible use to your oral surgeon regardless of the procedure’s complexity.
How Long Should You Stop Edibles Before Cosmetic Surgery?
You should stop edibles before cosmetic surgery at least one to two weeks in advance. Cosmetic procedures carry heightened concerns about bleeding, bruising, and wound healing, all areas where cannabinoids pose documented risks. THC and CBD both affect platelet aggregation and vascular tone, increasing the likelihood of excessive bruising or hematoma formation during facelifts, liposuction, or abdominoplasty.
Many cosmetic surgeons enforce stricter cessation timelines than other specialties because aesthetic outcomes depend heavily on clean healing. Edible cannabinoids also interfere with post-surgical pain management protocols, as regular users often require higher opioid doses for adequate relief. This two-week window allows CB1 receptors to resensitize and hepatic enzyme activity to normalize, giving your surgical team the most predictable pharmacological baseline.
With clear cessation timelines established, understanding what happens if you consume edibles too close to your procedure highlights why these windows matter.
What Happens If You Eat an Edible Too Close to Surgery?
Eating an edible too close to surgery increases risks related to anesthesia, bleeding, cardiovascular instability, drug interactions, and post-surgical recovery. The following subsections break down each complication category.
What Are the Risks of Increased Anesthesia Resistance?
The risks of increased anesthesia resistance include the need for significantly higher doses of anesthetic agents, which complicates dosing precision and prolongs sedation unpredictably. THC from edibles activates CB1 receptors in the brain, and chronic exposure desensitizes these receptors. This forces anesthesiologists to escalate medication to achieve adequate sedation depth. Because edibles produce prolonged, potent metabolites like 11-hydroxy-THC, the interference window extends well beyond the initial high. Underdosing risks awareness during surgery, while overcorrection risks respiratory depression. For patients who consume edibles regularly, this resistance creates a narrow and difficult-to-manage therapeutic window that puts surgical safety at stake.
What Are the Risks of Excessive Bleeding During Surgery?
The risks of excessive bleeding during surgery stem from cannabinoid effects on platelet function and vascular tone. THC can inhibit platelet aggregation, impairing the body’s ability to form clots at surgical sites. This becomes especially dangerous during invasive procedures where controlled hemostasis is critical. According to Michigan Medicine, people who use marijuana were more likely to experience complications, including higher stroke and bleeding risks, after heart procedures. Even for non-cardiac surgeries, the anticoagulant-like effects of residual THC metabolites from edibles can increase intraoperative blood loss and complicate wound closure. Surgeons often have limited ability to reverse these effects mid-procedure.
What Are the Risks of Heart Rate and Blood Pressure Changes?
The risks of heart rate and blood pressure changes involve unpredictable cardiovascular responses during surgery. THC increases heart rate through sympathetic nervous system activation while simultaneously causing vasodilation, which drops blood pressure. Under anesthesia, these opposing forces create hemodynamic instability that is difficult to manage. Edibles intensify this problem because their slower absorption produces sustained cannabinoid levels throughout a procedure. Anesthesiologists rely on predictable cardiovascular baselines to titrate medications safely; active THC metabolites disrupt that baseline entirely. For patients with underlying cardiac conditions, even mild instability during surgery can escalate into serious events. Disclosing edible use helps the surgical team prepare appropriate monitoring and intervention protocols.
What Are the Risks of Dangerous Drug Interactions?
The risks of dangerous drug interactions arise because cannabinoids inhibit the same liver enzymes responsible for metabolizing anesthesia drugs, opioids, and sedatives. According to a study published in the National Institutes of Health (PMC), delta-8-tetrahydrocannabinol results suggest a high risk of drug interactions, especially with oral use, due to its inhibitory effects on major hepatic enzymes. This enzyme inhibition can cause other surgical medications to accumulate to unsafe levels in the bloodstream, amplifying side effects or toxicity. Edibles pose a particularly high interaction risk because oral cannabinoids undergo extensive first-pass metabolism, producing metabolites that compete directly with pharmaceutical compounds for CYP450 processing.
What Are the Risks of Post-Surgical Nausea and Complications?
The risks of post-surgical nausea and complications include heightened postoperative nausea and vomiting, increased pain sensitivity, and greater opioid consumption during recovery. While cannabinoids have antiemetic properties at low doses, the paradoxical effect of chronic or recent heavy use can worsen nausea after anesthesia. Patients with active THC in their system also tend to report higher pain scores postoperatively, potentially requiring stronger pain management that carries its own risks. These compounding recovery challenges can extend hospital stays and delay return to normal activity. For anyone scheduled for surgery, stopping edibles within the recommended timeframe remains the most practical way to reduce these complications.
Should You Tell Your Doctor or Anesthesiologist About Edible Use?
Yes, you should tell your doctor or anesthesiologist about edible use before any surgical procedure. Full disclosure allows the anesthesia team to adjust dosing, anticipate drug interactions, and plan for potential cardiovascular or respiratory complications. Despite the importance of transparency, many patients withhold this information.
According to a 2024 study published by the National Institutes of Health, approximately 43.2% of medical cannabis users do not disclose their use to a primary care provider, with nearly 40% citing fear of provider disapproval as the reason. This nondisclosure creates a dangerous blind spot. Anesthesiologists who are unaware of cannabinoid use cannot account for the higher anesthetic doses, increased postoperative pain, or elevated nausea risk that cannabis users often experience.
Several reasons make honest disclosure essential:
- THC and CBD inhibit CYP450 enzymes, which metabolize many anesthetic and perioperative drugs, creating unpredictable drug interactions.
- Cannabis users may require significantly higher anesthesia doses, and without this knowledge, the surgical team cannot calibrate safely.
- Edibles produce the potent metabolite 11-hydroxy-THC, which lingers longer than inhaled THC and compounds interaction risks.
- Surgical teams are bound by confidentiality and cannot share medical disclosures with law enforcement, regardless of state cannabis laws.
Concerns about judgment from providers are understandable but largely unfounded in modern surgical settings. The conversation is clinical, not legal. Anesthesiologists need accurate information the same way they need to know about prescription medications, supplements, or alcohol use. Withholding edible use does not protect you; it removes a critical safety variable from the hands of the people responsible for keeping you stable during surgery.
For anyone who uses edibles regularly, proactive honesty during the pre-surgical consultation is one of the simplest steps toward a safer outcome. With anxiety alternatives and proper cessation timelines in place, the surgical team can build the safest possible plan.

What Are Safer Alternatives for Pre-Surgery Anxiety and Pain?
Safer alternatives for pre-surgery anxiety and pain include non-pharmacological relaxation techniques, topical CBD products, and doctor-approved medications. Each option carries a different safety profile depending on how close you are to your procedure.
What Non-Cannabinoid Relaxation Methods Can You Use Before Surgery?
Non-cannabinoid relaxation methods you can use before surgery include several evidence-based techniques that reduce preoperative anxiety without interfering with anesthesia. According to a 2022 review published in Frontiers in Public Health, non-pharmacological methods for reducing preoperative anxiety include cognitive-behavioral therapy, music therapy, aromatherapy, and guided imagery relaxation therapy.
These approaches work well because they carry no risk of drug interactions with surgical medications. Patients can practice guided breathing or listen to calming music in the hours leading up to a procedure, something no ingestible cannabinoid product can safely offer that close to surgery. For anyone accustomed to using edibles for relaxation, building familiarity with these techniques weeks before a scheduled operation makes the transition easier.
Can Topical CBD Be Used Safely Closer to Surgery?
Topical CBD can generally be used closer to surgery than oral edibles, though patients should still consult their surgical team first. Unlike ingested cannabinoids, topical CBD products penetrate skin layers for localized relief without producing significant systemic absorption. This means topical formulations are far less likely to inhibit CYP450 liver enzymes or interact with anesthesia drugs.
That said, “closer to surgery” does not mean “day of surgery.” Most anesthesiologists prefer patients disclose all cannabinoid use, including topicals, so the care team can make fully informed decisions. Applying a topical CBD cream several days before a procedure for localized discomfort is a reasonable middle ground, but stopping all forms at least 24 to 48 hours prior remains the safest practice.
What Doctor-Approved Medications Help With Pre-Surgery Anxiety?
Doctor-approved medications that help with pre-surgery anxiety include short-acting benzodiazepines, beta-blockers, and certain antihistamines prescribed specifically for the perioperative period. These medications have well-studied pharmacokinetic profiles, allowing anesthesiologists to account for them precisely when calibrating sedation.
Beyond pharmaceuticals, complementary approaches are gaining clinical support. A report from the National Center for Complementary and Integrative Health found that acupuncture therapy performed prior to surgery helps reduce preoperative anxiety in patients. Vitamin D supplementation has also shown favorable effects on anxiety levels, with higher blood concentrations within the normal range proving beneficial. Combining a prescribed anxiolytic with one of these complementary strategies often produces the best results, giving patients effective relief without the unpredictable drug interactions that cannabinoid edibles introduce.
With safer pre-surgery options identified, understanding how long cannabinoids remain detectable helps complete the picture.
How Long Do Cannabinoids from Edibles Stay in Your System?
Cannabinoids from edibles stay in your system for varying durations depending on the compound type and your usage pattern. THC metabolites persist longer than CBD, and chronic users retain detectable levels far longer than occasional consumers.
How Long Does THC from Edibles Stay in Your Body?
THC from edibles stays in your body longer than THC from inhaled cannabis. Oral administration of THC leads to higher concentrations of the metabolite 11-hydroxy-THC (11-OH-THC), which is more potent and longer-lasting than delta-9-THC, according to Pinnacle Recovery. This extended metabolic process means edible-derived THC produces effects that linger well beyond what smoking delivers.
Detection windows for THC metabolites in urine range from approximately 3 days for occasional users to more than 30 days for chronic, heavy users. Factors such as body fat percentage, hydration levels, and metabolic rate all influence how quickly your body eliminates these compounds. For anyone preparing for surgery, this extended clearance timeline makes early cessation essential.
How Long Does CBD from Edibles Stay in Your Body?
CBD from edibles generally stays in your body for 2 to 5 days in most users, though heavy or prolonged use can extend detection to several weeks. Because edible CBD undergoes extensive first-pass metabolism in the liver, its bioavailability is lower than inhaled forms, yet its metabolites can still accumulate in fatty tissue over time.
CBD’s unique pharmacological profile adds another consideration. Unlike THC, CBD does not attach to CB1 and CB2 receptors directly. Instead, it modulates endocannabinoid tone by hindering the uptake of anandamide. While this mechanism is subtler, CBD still interacts with the CYP450 enzyme system, which matters significantly when surgical medications enter the equation.
How Does Frequency of Use Affect Cannabinoid Clearance Time?
Frequency of use is the single most significant factor affecting cannabinoid clearance time. Occasional users typically clear THC metabolites within days, while daily or heavy users may require 30 days or longer to test negative.
Chronic cannabis use causes CB1 receptor down-regulation and desensitization, a process that begins reversing after 24 to 48 hours of abstinence but requires approximately 4 weeks to fully normalize, according to research published in Regional Anesthesia & Pain Medicine. This receptor recovery timeline explains why surgical guidelines emphasize extended cessation periods for regular users.
- Occasional users (once or twice monthly) generally clear cannabinoids within 3 to 7 days.
- Moderate users (several times weekly) may need 10 to 21 days for full clearance.
- Daily or heavy users often require 30 days or more before metabolites become undetectable.
Understanding your own usage frequency helps you plan a realistic cessation timeline well ahead of any scheduled procedure.
What Should You Know About Resuming Edibles After Surgery?
Resuming edibles after surgery requires careful timing, medical clearance, and awareness of how cannabinoids interact with recovery. The following subsections cover safe timelines, pain management potential, and which cannabinoids best support post-surgery wellness.
How Long After Surgery Is It Safe to Use Edibles Again?
It is generally safe to use edibles again once your surgeon confirms that anesthesia has fully cleared your system, you are no longer taking interacting medications, and initial wound healing has progressed. For most patients, this means waiting at least 48 to 72 hours after minor procedures and potentially one to two weeks after major surgery. THC and CBD both inhibit CYP450 liver enzymes, so reintroducing edibles while still on prescription painkillers or blood thinners can alter drug metabolism unpredictably. Starting with a low dose after clearance is the safest approach, since post-surgical physiology may amplify cannabinoid effects compared to your pre-surgery tolerance.
Can Edibles Help With Post-Surgical Pain and Recovery?
Edibles can help with post-surgical pain and recovery for some patients, though evidence remains mixed. Cannabinoids interact with the body’s endocannabinoid system to modulate pain signaling and inflammation. However, according to a 2025 update from the Anesthesia Patient Safety Foundation, cannabis users demonstrate increased postoperative opioid consumption and higher pain scores compared to non-users. This suggests that regular cannabinoid use before surgery may actually complicate pain management afterward. For someone resuming edibles specifically for recovery support, occasional low-dose use under medical supervision is more practical than daily high-dose consumption, which risks tolerance buildup and diminished analgesic benefit.
Which Cannabinoids Are Best Suited for Post-Surgery Wellness?
The cannabinoids best suited for post-surgery wellness are CBD and low-dose THC, each offering distinct recovery benefits through the endocannabinoid system. According to the Anesthesia Patient Safety Foundation, cannabinoids act as partial agonists on CB1 and CB2 G-protein coupled receptors located throughout the body and brain. CBD supports anti-inflammatory and anxiolytic effects without intoxication, making it suitable during active recovery. Low-dose THC may aid sleep and appetite stimulation when healing demands increase. Delta-8 THC carries a higher drug interaction risk due to hepatic enzyme inhibition, so it warrants extra caution during the medication-heavy post-operative window. Always confirm cannabinoid use with your prescribing physician before reintroducing any product.
With post-surgery resumption guidelines in mind, choosing quality products matters most.
How Can You Choose Quality Hemp-Derived Edibles for Your Wellness Routine?
You can choose quality hemp-derived edibles by prioritizing third-party lab testing, verified cannabinoid content, and federal compliance. The sections below cover how IndaCloud meets these standards and summarize key takeaways about stopping edibles before surgery.
Can IndaCloud’s Lab-Tested Hemp Edibles Support Your Recovery Goals?
Yes, IndaCloud’s lab-tested hemp edibles can support your recovery goals when used at appropriate times outside surgical windows. IndaCloud subjects every product to comprehensive third-party testing, verifying cannabinoid potency and purity across its full edible lineup, including gummies, baked goods, and functional popping crystals. All products contain less than 0.3% Δ9-THC, maintaining 100% federal legality.
For post-surgical wellness specifically, choosing edibles with verified lab reports matters because cannabinoid content directly affects how these compounds interact with your body’s endocannabinoid system. IndaCloud organizes products by desired effect, such as relaxation or focus, helping users select options aligned with their recovery stage. With over 250,000 verified customers and a team of 35 cannabis experts backing product development, IndaCloud provides the transparency and quality assurance that wellness-conscious consumers need when reintroducing hemp-derived edibles after medical clearance.
What Are the Key Takeaways About Stopping Edibles Before Surgery?
The key takeaways about stopping edibles before surgery center on timing, transparency, and patient safety. Always disclose cannabinoid use to your surgical team; according to a 2023 study published by the National Institutes of Health, approximately 43.2% of medical cannabis users do not disclose their use to a primary care provider, creating preventable risks.
Essential points to remember include:
- THC edibles require longer cessation windows than smoked cannabis because oral THC produces higher concentrations of the potent metabolite 11-hydroxy-THC.
- Most clinical guidelines recommend stopping edibles at minimum 72 hours before surgery, with heavier users needing longer abstinence periods.
- Cannabinoids interact with the CYP450 enzyme system, potentially altering how your body processes anesthesia and other surgical medications.
- Safer pre-surgery alternatives exist, including cognitive-behavioral therapy, music therapy, and doctor-approved anxiolytics.
- After surgery, resume edibles only with your physician’s clearance, starting at lower doses to account for post-operative medication interactions.
Planning ahead and communicating openly with your healthcare team remain the most reliable ways to ensure both surgical safety and a smoother recovery.